By Scott Brown, Optometrist | Scotlens Clinical Director & Lens Designer
Given the growth of Ortho-K night lenses and soft lenses being used for myopia control, in this article I focus on what we can do when teaching application and removal (A&R) in order to get kids started with contact lenses successfully. I especially want to highlight the fact that dropout rates go from 1 in 20 when anaesthetic is used for A&R, compared to 1 in 5 without!1. Although focused on kids, this information is applicable for all ages.
Teaching kids (of any age) Application & Removal
ECPs are seeing younger patients than they may have been used to due to the increased demand for ortho-k night lenses and myopia control day lenses. As an NHS contact lenses fitter I am referred patients that ‘need’ contact lenses in order to lead a normal life. These patients are not always keen on contact lenses, so I not only need to get them fitted with an appropriate lens, but also need to make the fitting process a positive experience, converting the opinions of a reluctant patient. Here are some tips that can be beneficial for all new contact lens wearers.
With night lenses (or any GP) ALWAYS use anaesthetic the first time the patient will have the lenses on their eyes.
“I wore them for years, they are not that bad, they will need to get used to them”
This is often the mantra of the older generation of ECPs that teach contact lens fitting today. Years ago there was much less choice, so patient motivation was higher and they would put up with what they were given. GPs are “not that bad”, but the subjective comfort varies between patients, some being much more sensitive before they become adapted. Adapted comfort is good, but it may take patients a few weeks to get there. They do “need to get used to them”, but the purpose of the application & removal appointment is to learn handling, NOT adaption. If patients are distracted by lens awareness they will not focus on your instructions.
“I don’t have a problem teaching folk without anaesthetic”
Another statement I often hear. Communication and experience certainly can make this statement true, but it does not make the first impressions for the patient any better. Drop out when anaesthetic is used the first time the patient experiences GP lenses in is 1 in 20, without anaesthetic it is is 1 in 5!1 So first impressions last! Again, the purpose of the A&R is to learn handling, not to become adapted.
“Drops sting as much as the lenses”
I use proxymetacaine and have it a room temperature, which means it does not nip. If you use benoxinate try them on yourself and then see which one you would rather have put in! They both are better than none, but proxy gives a better patient experience.
Do you always use anaesthetic?
Yes, always for at least one eye. If I have an experienced wearer moving to night lenses from softs I will anesthetise the first eye. Teach the A&R ideally getting three applications and removals.
- I will highlight there is almost no lens sensation when the lens goes in first.
- I reinforce this is what the lenses will feel like when the eyes are open and blinking in just a few weeks.
- By the third application the anaesthetic is wearing off and I can highlight that the comfort is good when the eye is closed, and that it is only when blinking that the lens will be felt.
Not feeling the lens with the eyes closed is why patients have no issues adapting to night lenses, compared to daytime GPs where adaption takes a good few weeks.
With an experienced wearer, or, if A&R is good, I may not use anaesthetic for the second eye so the patient will know what the lens will feel like when they try it at home. But supervised handling and more successful A&R practice is the priority over the patient experiencing the lens.
I make sure the patient expects
- There will be more lens sensation when at home and that it is normal
- It will be minimal once the eyes are closed
- That it will improve to the point where they don’t feel the lenses with time
Appointment requirements for kids under 12
I assume for younger kids I will need two A&R appointments. I tell all my patients they will need two anyway, that way they are not disappointed if they don’t manage and they feel proud if they manage in the first appointment.
Soft lenses
Soft lens application can also be made easier with anaesthetic as it calms the blink reflex and can often allow successful application when a twitchy lid prevents it. This can give a demoralised patient the confidence they will manage with a bit more practice and time.
Don’t be reluctant to use a sucker!
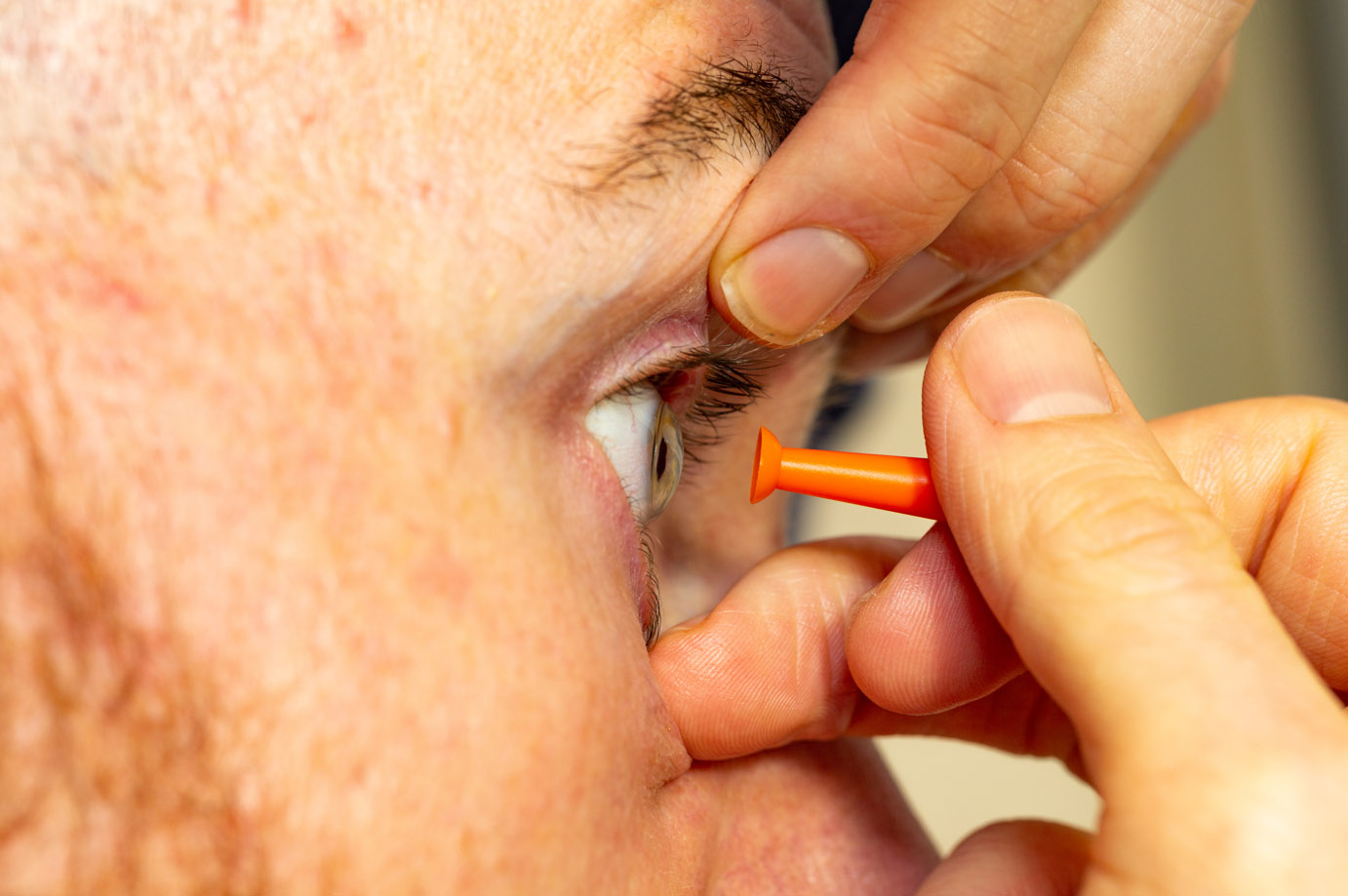
Suckers should always be supplied with GPs to enable lifting the lens up off a counter or sink if dropped to prevent lens damage. They should not be used for lens insertion with the exception of scleral type lenses.
I always try to teach patients application with the lens on a fingertip, a drop of solution in the lens bowl, keeping their hand still and then looking down onto the lens. Small fingers often need to balance the lens in between two fingers (middle and pointing) as it will just keep falling off once a drop of solution is applied.
Removal is with the tiddly wink lid pinch. This is ultimatetly what I want patients to be able to do. However, it is more important in the limited appointment time, that the patient gets as much practice as possible and can apply and remove the lenses in a safe manner. When new to contact lenses, this may not be the best technique. It may be that a parent needs to help, or they may have to use a sucker to remove. There is a lot of information for patients to absorb. So, work out what is going to be safe to get the patient started, then instruct the best techniques in a couple of weeks time when they are familiar with lens wear.
The infection risk of suckers
Suckers pose little infection risk as they are used only to touch the lens as it is removed and then cleaned. They are made of silicone and do not absorb contaminants, so instruct patients to keep them clean in the same way they do their lens case.
[SCOTLENS VIDEO GUIDE: “Different types of suckers” – click here to view]
Go straight to teaching your patient.
Remember your patient will be nervous about having to poke their finger in their eye for the first time.
“Are you feeling nervous? Don’t worry, everybody does, we are not meant to want to poke our eyes!”
A simple comment like this lets them know you understand how they feel, and can help put patients at ease.
Then go straight to instructing them on the A&R. There is no advantage to you showing the patient you can put the lenses in their eye, as they need to learn they can do it themselves. If they can’t manage by the end of the appointment, and you think showing them the vision they will get will motivate them for the next appointment, put the lenses in for them. Otherwise, they will learn nothing from you putting the lenses in for them. With custom fit GPs or soft lenses, the fit assessment is the second priority of the A&R appointment. It can usually be quickly assessed after application is learned at the end of the appointment. Any changes to lens fit or power can be changed either at the end, or for the lenses being supplied for the home trial.
Always try to get the patient to leave feeling they having achieved some progress, even if they need to come back to have more practice before getting the lenses home.
- Bennett, E.S.,et al (1998) “The effect of topical anesthetic use on initial patient satisfaction and overall success with rigid gas permeable contact lenses”. Optom. Vis. Sci. 75 (11): 800-805.




